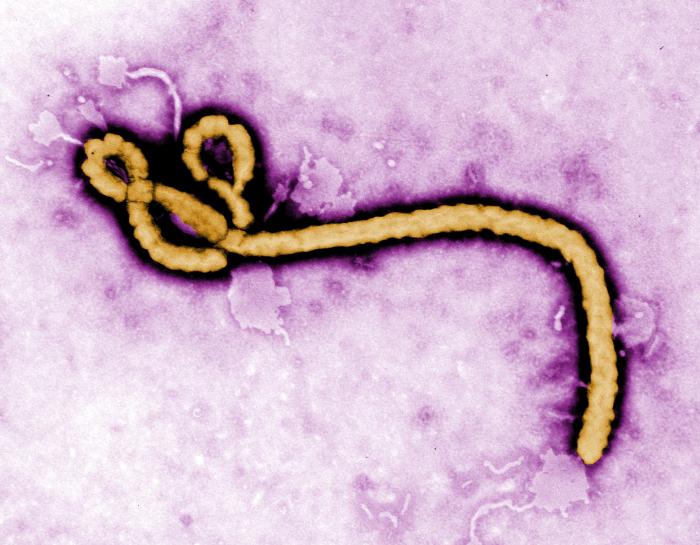
 Two Ebola virus disease cases have been identified among healthcare workers in Texas, underscoring the importance of maintaining strict adherence to infection control precautions when working with Ebola patients. We know that the general public in the US isn’t at risk – but we also know that healthcare workers have the highest risk. The good news is that the risk of transmission can be dramatically reduced as long as certain protocols and procedures are followed. This means following them at the structural level (i.e. the treating facility), the clinical team level, and the individual level. With this many levels of possible breakdown it can be challenging to fully protect workers. But it’s entirely possible – after all Doctors Without Borders has been doing it successfully for months now in West Africa.
Two Ebola virus disease cases have been identified among healthcare workers in Texas, underscoring the importance of maintaining strict adherence to infection control precautions when working with Ebola patients. We know that the general public in the US isn’t at risk – but we also know that healthcare workers have the highest risk. The good news is that the risk of transmission can be dramatically reduced as long as certain protocols and procedures are followed. This means following them at the structural level (i.e. the treating facility), the clinical team level, and the individual level. With this many levels of possible breakdown it can be challenging to fully protect workers. But it’s entirely possible – after all Doctors Without Borders has been doing it successfully for months now in West Africa.
CDC has checklists for hospitals, healthcare facilities, healthcare providers, and EMS to facilitate readiness and gap assessments for healthcare professionals. If presented with a patient experiencing fever or other Ebola symptoms, healthcare providers should take the following steps:
- Inquire about a history of travel to West African countries with Ebola outbreaks (Guinea, Liberia, and Sierra Leone) in the 21 days before illness onset for any patient presenting with fever or other symptoms consistent with Ebola;
- Immediately isolate a patient who reports a travel history to an Ebola-affected country (currently Liberia, Sierra Leone, and Guinea) and who is exhibiting Ebola symptoms in a private room with a private bathroom and implement standard, contact, and droplet precautions (gowns, face mask, eye protection, and gloves);
- Notify your local health department. The local public health department will help to evaluate risk, coordinate with the ADHS and help to arrange for specimen shipment and testing at the ADHS Lab (if warranted);
- If testing is warranted based on consultation with public health, ensure all proper personal protective equipment and precautions for collecting a blood borne pathogen sample are followed;
- Maintain a log tracking all people in contact with the patient, including visitors, healthcare workers, environmental services, and others. Infection prevention and environmental control guidelines must be followed to protect staff and other patients;
- Healthcare workers treating an Ebola virus disease patient should monitor their temperature twice a day for 21 days. Most healthcare workers who treat Ebola patients will never contract it themselves, but it’s important to be vigilant as a precaution; and
- There is no specific FDA approved treatment for Ebola virus disease but supportive care can greatly benefit patient recovery. CDC has some treatment information on their website.
Throughout the course of patient treatment, it’s critical that healthcare facilities follow all personal protective equipment guidance. We’ve learned from other hospitals who have treated Ebola patients that having a 24/7 site manager to monitor protective equipment including donning and doffing is critical. Other facilities have had success using the buddy system to double check methods. Practicing proper donning and doffing will help ensure appropriate use in the event an Ebola patient does present at your facility.
Communication between direct-care workers and systems level workers are keys for success. Assessing your readiness and following the CDC guidance are crucial to reducing likelihood of disease spread.